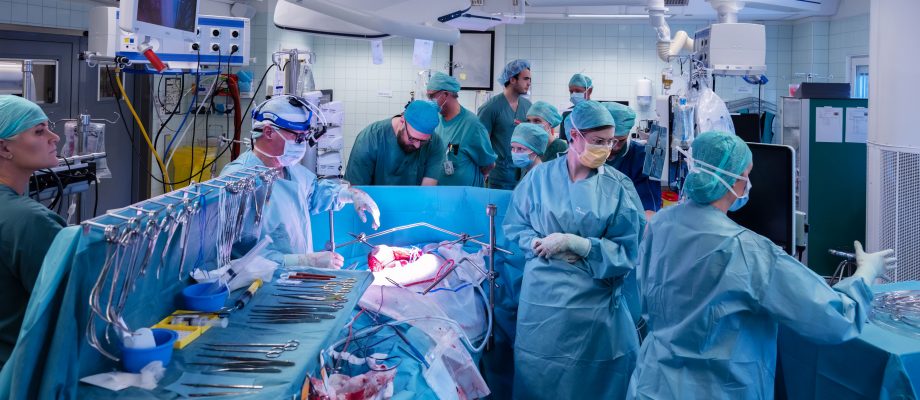
NEW STUDY. An advanced surgical therapy has proved considerably more efficacious than conventional treatments for patients with melanoma in the eye (uveal) that has spread to the liver, a University of Gothenburg study shows. The treatment involves perfusing the liver with very high doses of chemotherapy.
Melanoma in the eye (uveal) is an unusual form of melanoma that arises not in the pigment cells of the skin but in the eye. In Sweden, some 80 people are diagnosed with the disease annually. In half of the patients, this form of cancer causes liver metastases, which entail a highly unfavorable prognosis. After metastases in the liver have been found, a large majority of patients die within one year. Unfortunately, current treatments with immunotherapy or chemotherapy have only very limited effects.
The new results are published in the Journal of Clinical Oncology. In the study, 87 patients with metastasized uveal melanoma were assigned to receive either the established treatment regarded by the patient’s doctor as the best option, or the present experimental therapy, known as “isolated hepatic perfusion” (IHP).
Tumors shrank in 40 percent of patients
In the group undergoing IHP treatment, the subsequent X-ray examination showed that the tumors had shrunk in 39.5 percent of patients compared to only 4.5 percent of the patients in the group receiving conventional treatment.

“This is the first therapy that’s been shown to shrink tumors as effectively for this group of patients. Our long-term goal is to enable the patients to become cancer-free, but to date we haven’t been able to say that the treatment can cure the patients,” says Professor Roger Olofsson Bagge of the University of Gothenburg and senior consultant surgeon at Sahlgrenska University Hospital.
The study and treatment method have aroused keen interest worldwide. Discussions at an international level will potentially lead to the new treatment being the one recommended for this patient category.
Major operation
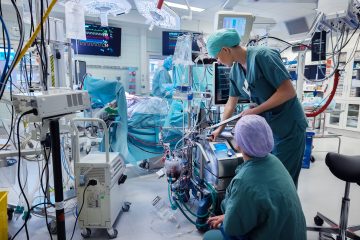
The IHP procedure is a large-scale surgical intervention involving open surgery in which the liver is surgically isolated and connected to a heart-lung machine. Extremely high doses of a chemotherapeutic agent is then pumped through the lever for one hour, after which all the chemotherapy is flushed away and the liver reconnected to the patient’s own circulation. Using this method, it is possible to administer an extremely high dose of chemotherapy concentrated to the part of the body that harbors the cancer cells, while the rest of the body do not get any negative effect.
“It’s a major operation involving open surgery, but next year we’ll be starting to use a minimally invasive method where the liver is isolated with balloons inserted into the blood vessels of the groin,” Olofsson Bagge says.
Only in Gothenburg
Since this form of cancer is so unusual, it has taken nearly ten years to complete the clinical phase III study. Almost all of Sweden’s university hospitals have contributed patients to the study, but the actual IHP treatment has been implemented at Sahlgrenska University Hospital.
The treatment was developed in the U.S. back in the 1960s. It has been tested for a number of tumor diseases, but only now has a study succeeded in showing how efficacious the therapy is specifically for patients with uveal melanoma that has metastasized (spread) to the liver.
Title: Isolated Hepatic Perfusion with Melphalan for Patients with Isolated Uveal Melanoma Liver Metastases: A Multicenter, Randomized, Open-Label, Phase III Trial (the SCANDIUM trial); DOI
BY: ELIN LINDSTRÖM
Bara i Göteborg
Eftersom cancerformen är så ovanlig har det tagit närmare tio år att genomföra den kliniska fas III-studien. Nästan alla universitetssjukhus i Sverige har bidragit med patienter till studien, men själva IHP-behandlingen har genomförts på Sahlgrenska Universitetssjukhuset.
Behandlingen utvecklades i USA redan under 1960-talet. Den har testats för ett flertal olika tumörsjukdomar, men det är först nu som en studie kunnat visa hur pass effektiv behandlingen är för just patienter med ögonmelanom som spridit sig med dottertumörer till levern.
AV: ELIN LINDSTRÖM
FOTO: PAUL BJÖRKMAN/SAHLGRENSKA UNIVERSITETSSJUKHUSET